Anatomy of Uveal Tract: Choroid
Describes choroidal anatomy, layers, retinal interface, and uveal vascular supply and BRB details.
Choroid is a thin but highly vascular membrane lining the inner surface of sclera. It extends from anteriorly ora serrata to the optic nerve posteriorly. It has a rough outer surface which is attached to sclera at the optic nerve and at the exit of the vortex veins. The smooth inner surface of choroid is attached to the retinal pigmented epithelium (RPE). Choroid becomes continuous with pia and arachnoid at the optic nerve. Choroid is normally 100-220 µm thick; thickness is highest at macula 500- 1000 µm.
- Choroidal thickness increases in intraocular inflammation.
- The smooth configuration of the choroid can be observed ophthalmoscopically in choroidal detachment
Microscopic Structure of Choroid:
Choroid is composed predominantly of blood vessels surrounded by melanocytes, nerves and connective tissue. Choroid can be divided into the following layers histologically:
1. Suprachoroid lamina (lamina fusca):
Suprachoroid lamina is consist of collagen fibres, fibroblasts and melanocytes. Suprachoroid lamina overlies a potential space between sclera and choroid known as suprachoroidal space. This potential space contains the long posterior ciliary arteries and nerves.
2. Choroidal stroma:
Unlike tissues like iris, where stroma occupies a major part of the tissue, choroidal stroma is sparse as major bulk of choroid is made up of choriocapillaris. The choroidal stroma is a pigmented loose connective tissue which contains following elements:
- Vessels: The vessels of choroid are arranged in layers. Larger vessels are located on the outer side and the layer is called Hallers layer. The vessels of this layer branch and form medium sized vessels. The layer of these medium sized vessels are known as Sattler's layer. These vessels again branch forming smaller vessels and capillaries. Venues of choroid drain to veins which ultimately drain to four vortex veins (one from each quadrant of the eye).
Choroidal veins are devoid of valve
- Nerves:
- Cells: Melanocytes, fibrocytes, mast cells and plasma cells are the predominant cells found in choroidal stroma. Melanocytes are distributed heavily in outer part of the layer and near optic disc. Among the non-pigmented cells, fibroblasts are the most common.
- Connective tissue: Collagen fibrils are dispersed in all directions and surround the blood vessels
3. Layer of Choriocapillaris:
It is a single layer of capillaries which are larger than the normal capillaries of our body. It has been estimated that the lumen of these capillaries are three to four times larger than normal capillaries. The capillary walls are fenestrated and contains pericytes. Choriocapillaries contain a basement membrane.
Pericytes found in capillaries are also known as cells of Rouget. They have the contractile functions and are believed to alter the blood flow in capillaries.
Choriocapillaries are thickest and most abundant in submacular area. Experimentally it has been found that choriocapillaries are arranged in lobular structure where the feeding arterioles are in the centre and draining veins are in the periphery.
Choroidal circulation: tits bits
- Choroidal circulation constitutes 85% of the blood circulation of the eye.
- Choroidal blood flow is higher than that in tissues like retina and brain.
- Choroidal blood-flow range from 800 to 2000 mL/min/100 g of tissue.
- Choroid provides the metabolic requirements of the full retinal thickness only in the macular region.
- In embryonic life, choroid serves as an additional site for the erythropoiesis.
4. Bruch's membrane:
Bruch's membrane are the innermost layer of choroid and it is also known as lamina vitrea. Bruch's membrane is thickest near optic disc (2-4 microm) and the thickness decreases towards periphery. Bruch's membrane is composed of 5 layers and from internal to external, these are
- Basement membrane of the RPE,
- Inner collagenous zone,
- Elastic tissue layer,
- Outer collagenous zone, and
- Basement membrane of the choriocapillaris

Outer blood–retinal barrier
The outer blood–retina barrier (BRB) is composed of three structural entities, the fenestrated endothelium of the choriocapillaris, Bruch's membrane, and the retinal pigment epithelium (RPE).
|
Iris |
Ciliary body |
Choroid/ Retina |
|
Supra ciliary lamina |
||
|
Stroma |
||
|
BM of the anterior iris epithelium |
BM attaches the pigment epithelium to the stroma |
BM of Bruch's membrane of the choroid |
|
Anterior epithelium of iris |
Pigment epithelium |
Retinal pigment epithelium |
|
Posterior pigment epithelium of iris |
Non pigment epithelium |
Sensory retina |
|
Internal limiting membrane |
Internal limiting membrane |
Blood supply of uveal tract:
The blood supply of the uveal tract is mainly from three arteries namely short posterior ciliary arteries, long posterior ciliary arteries and anterior ciliary arteries.
The posterior ciliary arteries are branches of the ophthalmic artery, and much variation can occur in their distribution.
Short Posterior Ciliary Arteries
15 to 20 short posterior ciliary arteries arise → form 10 to 20 branches → enter the sclera in a ring around the optic nerve → anastomose with other branches from the short posterior ciliary arteries to form the circle of Zinn (Zinn-Haller) which encircles the optic nerve at the level of the choroid → they run in suprachoroidal space between sclera and choroid, branch and supply the choroid.
Long Posterior Ciliary Arteries
Two long posterior ciliary arteries enter the sclera: one lateral and one medial to the ring of short ciliary arteries → run between the sclera and the choroid to the anterior globe → enter the ciliary body and branch superiorly and inferiorly → anastomose with each other and with the anterior ciliary arteries to form a circular blood vessel, the major arterial circle of the iris.
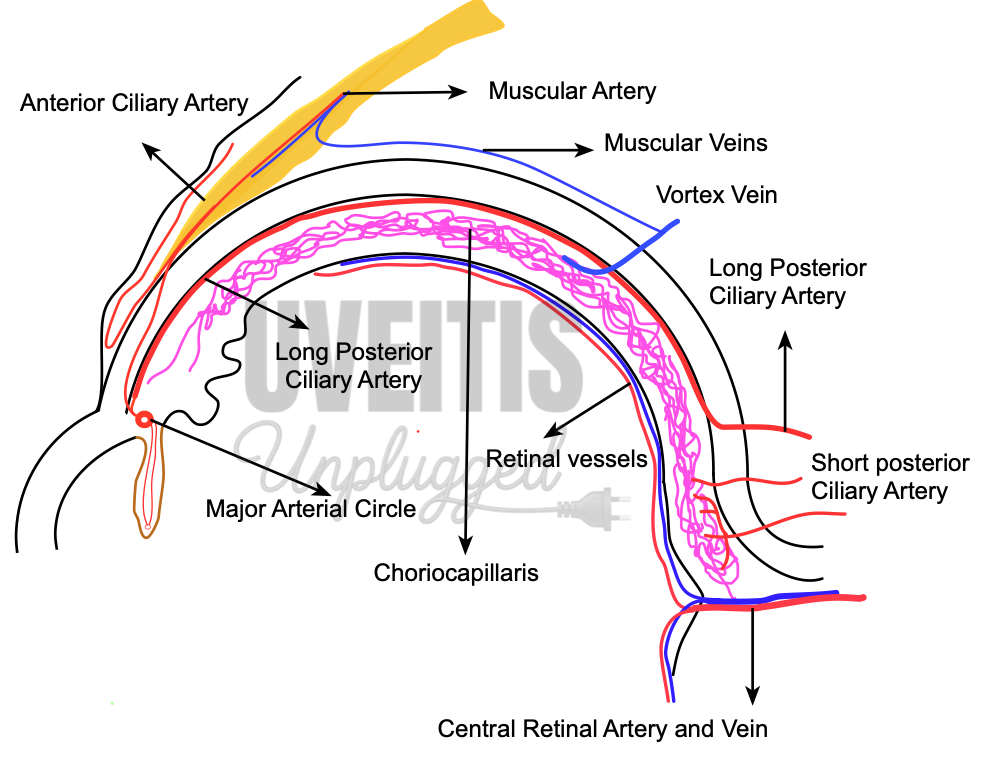
Anterior Ciliary Arteries
7 anterior ciliary arteries are derived from muscular branches of ophthalmic artery ( two each from arteries of superior rectus, medial rectus, inferior rectus and only one from lateral rectus muscle) → reaches episclera, form plexus and give branches →pierce sclera near the limbus to enter the eye → anastomoses with long posterior ciliary arteries to form major arterial circle of iris
Branches from major arterial circle enter iris and anastomoses with each other to form minor arterial circle.

